Understanding diabetes and oral health
Diabetes isn’t a choice, but we can choose the best strategy to fight it, especially when it comes to your dental health.
Nearly 30 million people battle diabetes, and every 23 seconds, someone new is diagnosed with diabetes.
Facts about diabetes and oral health

Here are some key facts about diabetes and oral health:
The connection between diabetes and oral health
Diabetes and oral health conditions are often related, according to the National Institute of Dental and Craniofacial Research. Patients with Type I or Type II diabetes are at an increased risk of developing tooth decay, gum disease, dry mouth, and various fungal infections in the mouth.
Fortunately, people with diabetes today can take a proactive approach to managing their oral health by following and controlling their glucose levels, practicing thorough oral hygiene, and visiting the dentist regularly for examinations and dental cleanings is important.

Oral health issues of uncontrolled diabetes
The immune system can easily become impaired when diabetes is not controlled. People with diabetes face a higher risk of oral health problems, such as:
1. Thrush
Those with diabetes who often take antibiotics to fight various infections in their body are most prone to developing a fungal infection of the mouth or tongue. The fungus thrives on the increased glucose levels in the saliva of people with uncontrolled diabetes.
Wearing dentures, especially if worn continually can be a great contributor to fungal infections.
People with diabetes who smoke are a much higher risk — up to 20 times more likely than non-smokers to develop thrush and periodontal disease. Smoking also is believed to impair blood flow to the gums, which could negatively impact the healing around the tissue or wound areas.
2. Burning mouth
A burning sensation in the mouth or tongue is caused by the presence of “thrush.”
3. Dry mouth
Unmanaged diabetes will often decrease saliva production which is the body’s way of naturally rinsing the mouth of harmful bacteria, resulting in dry mouth. Dry mouth, if untreated leads to infections, tooth decay, ulcers, and soreness in the mouth, jaw, and sinus cavity.
4. Periodontitis, gingivitis (gum inflammation)
Another complication of diabetes if left unchecked is the weakening of white blood cells which results in the thickening of blood vessels. This results in slowing the flow of nutrients to and waste products from the body tissues, including the mouth. This combination of events makes it difficult for the body to fight off infections.
Since periodontal disease is a bacterial infection, people with uncontrolled diabetes might experience more frequent and more severe gum disease.
5. Gum infection
Research also indicates that having a severe gum infection can make it much more difficult for diabetics to control blood sugar levels. If blood sugar is poorly managed, it is more likely that other oral health problems will arise.
6. Insufficient healing of oral tissues
Uncontrolled diabetes in a person can be a detriment to the proper healing of the oral tissues from dental treatments or oral surgery. This is due to the lack of blood flow to the surgical or area of therapy.
Are people with diabetes at a greater risk for dental cavities?
There are some who argue that elevated levels of glucose in the saliva of individuals with uncontrolled diabetes create a favorable environment for bacterial proliferation. Consequently, this leads to the emergence of gum disease and dental caries.
What is dental caries?
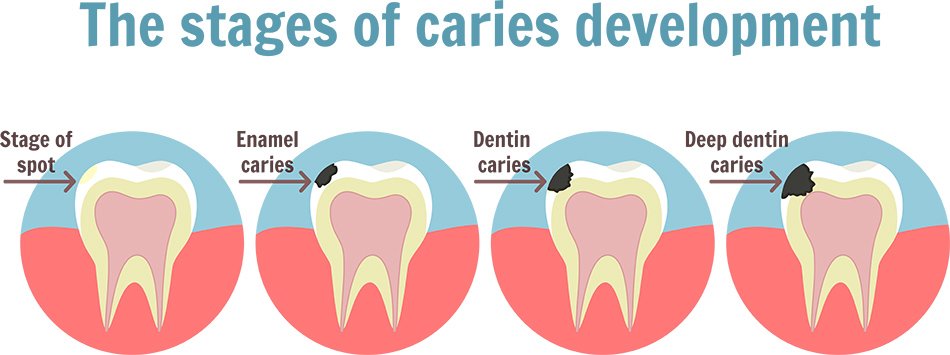
Dental caries, also known as tooth decay or cavities, is the breakdown of teeth due to acids made by bacteria. Here are some key facts about dental caries:
Additionally, individuals with diabetes often consume food more frequently throughout the day, thereby augmenting the likelihood of bacterial growth and the occurrence of cavities.
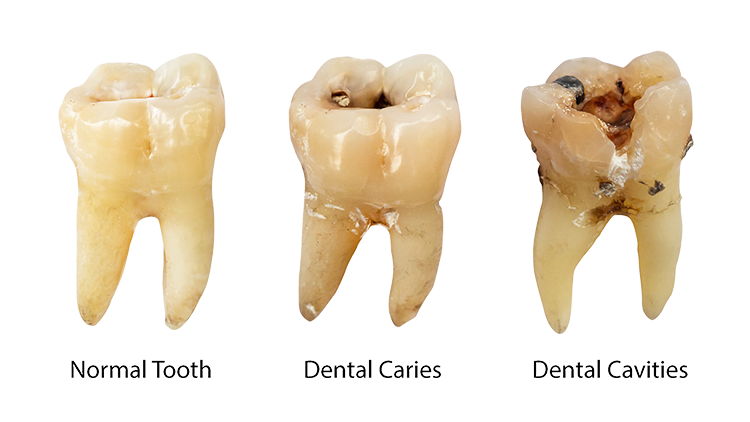
Some argue that individuals with diabetes have a heightened awareness regarding sugar management, leading them to consume fewer cavity-causing sugary foods.
Maintaining proper oral hygiene and a balanced blood sugar level are essential for protecting against cavities and periodontal disease.
What actions should individuals with diabetes take to maintain the health of their oral cavity and gums?
Given the heightened susceptibility of individuals with diabetes to infections and oral health issues, it is crucial to uphold proper oral hygiene practices and promptly address any oral health changes. Should any alterations arise, it is imperative to immediately seek dental attention.
11 Recommendations to Reduce and Prevent Oral and Dental Health Issues
Following are my recommendations to reduce or even prevent oral and dental health issues:
Diabetes is a disease that can affect the entire body — your eyes, heart, nerves, kidneys, and your teeth, gums, and mouth. With attention to medical care, awareness, and self-care that monitors and keeps blood sugar as close to normal as possible, and excellent personal and professional dental care, problems after dental treatments or oral surgery are no more likely in people with diabetes than in those without the disease.
